- Migraine Science
Cannabis for Migraines: What Science Says About Relief

Contents
Contents
If you’ve ever spent a day locked in a dark room waiting for a migraine to pass, you already know how limited your options feel. Over-the-counter painkillers barely touch it, and prescription triptans come with side effects that sometimes rival the migraine itself. A growing body of research now points to cannabis as a viable alternative for migraine sufferers, and the science behind it is more compelling than most people realize.
Cannabis migraines research has accelerated in the past five years. Studies from institutions like the National Institutes of Health and peer-reviewed journals have begun documenting what migraine patients have reported anecdotally for decades: cannabis can reduce both the frequency and severity of migraine attacks. This article breaks down the current evidence, the mechanisms involved, and what you should know before trying it yourself.
The endocannabinoid system and migraines
To understand why cannabis works for migraines, you need to understand the endocannabinoid system (ECS). This network of receptors and neurotransmitters runs throughout your brain and body, regulating pain perception, inflammation, mood, and immune responses.
The ECS has two primary receptor types: CB1 receptors, concentrated in the brain and central nervous system, and CB2 receptors, found mainly in immune cells and peripheral tissues. Both play roles in how your body processes pain signals. When the ECS functions normally, it produces endocannabinoids like anandamide and 2-AG that keep inflammation and pain signaling in check.
Here’s where migraines enter the picture. Dr. Ethan Russo, a neurologist and cannabis researcher, proposed the “Clinical Endocannabinoid Deficiency” (CED) theory in a paper published in Neuroendocrinology Letters. The theory suggests that chronic migraines, fibromyalgia, and irritable bowel syndrome may all stem from an endocannabinoid deficiency. Essentially, your body doesn’t produce enough of its own cannabinoids to regulate pain properly.
A 2020 review published in the Journal of Headache and Pain found supporting evidence for this hypothesis. Migraine patients in the study had lower levels of anandamide in their cerebrospinal fluid compared to healthy controls. If the CED theory holds up, supplementing with plant cannabinoids could address a root cause of migraines rather than just masking symptoms.
What the clinical research actually shows
The research on cannabis for migraines isn’t just theoretical. Several clinical studies have produced concrete numbers that migraine sufferers should pay attention to.
A landmark 2016 study from the University of Colorado followed 121 migraine patients who used cannabis. The results were striking: migraine frequency dropped from an average of 10.4 headaches per month to 4.6. That’s a 55.7% reduction. Nearly 40% of participants reported positive effects, with 19.8% saying cannabis helped prevent migraines entirely and 11.6% reporting it stopped migraines already in progress.
A 2019 study published in the Journal of Pain used data from the Strainprint app to analyze over 12,000 sessions where patients used inhaled cannabis for headaches and migraines. Headache severity dropped by 47.3% and migraine severity by 49.6%. However, the researchers noted that patients needed increasing doses over time, which suggests tolerance may develop.
More recently, a 2021 Israeli study published in Brain Sciences tracked 145 medical cannabis patients with migraines over three years. Monthly migraine days decreased from 8.1 to 4.1, and the patients also reported improvements in sleep quality and reduced reliance on prescription medications.
✓ Key research findings
- ✓ 55.7% reduction in monthly migraines (University of Colorado, 2016)
- ✓ 49.6% decrease in migraine severity with inhaled cannabis (Journal of Pain, 2019)
- ✓ Monthly migraine days cut in half over 3 years (Brain Sciences, 2021)
- ✓ Reduced dependence on prescription migraine medications
How cannabis compounds target migraine pain
Cannabis contains over 100 cannabinoids and dozens of terpenes, and several of them have specific mechanisms that are relevant to migraine pain. Understanding these helps explain why cannabis works differently than standard painkillers.
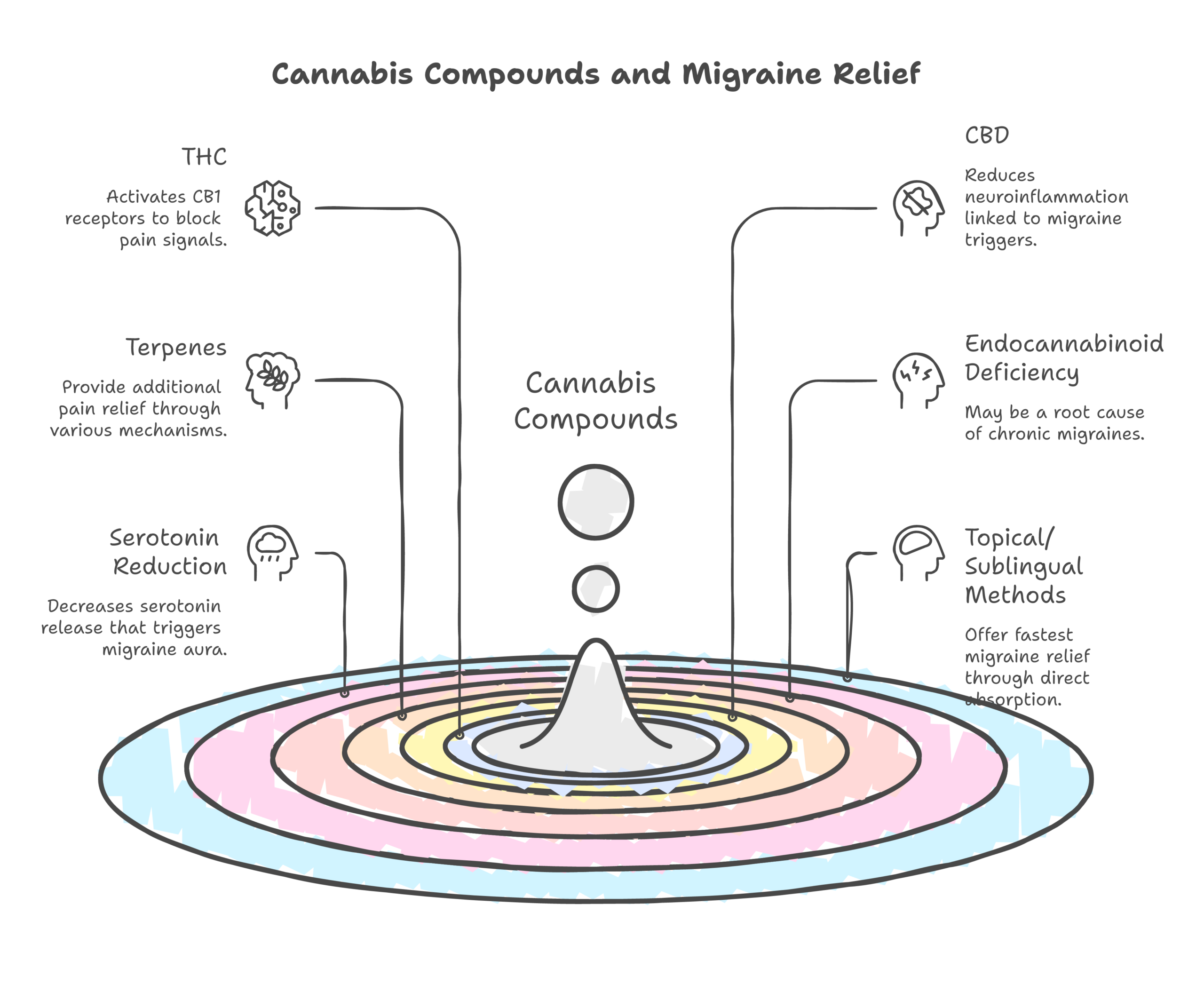
THC (tetrahydrocannabinol) binds directly to CB1 receptors in the brain’s pain processing centers, including the periaqueductal gray and the trigeminal nucleus. The trigeminal nerve is central to migraine pathology, as Mayo Clinic researchers have noted. When THC activates CB1 receptors in these areas, it dampens the pain signals that would otherwise escalate into a full migraine. THC also affects serotonin release, which is significant because serotonin fluctuations are a known migraine trigger.
CBD (cannabidiol) takes a different approach. Rather than binding directly to cannabinoid receptors, CBD inhibits the enzyme FAAH that breaks down anandamide. By keeping anandamide levels elevated, CBD may address the endocannabinoid deficiency that researchers believe contributes to chronic migraines. CBD also has documented anti-inflammatory properties, according to research published in Antioxidants journal, which helps because neuroinflammation plays a direct role in migraine pathogenesis.
Terpenes contribute to what researchers call the “entourage effect.” Myrcene, found in many cannabis strains, has analgesic and sedative properties. Linalool, also present in lavender, has shown anti-inflammatory effects in preclinical studies. Beta-caryophyllene is unique because it actually binds to CB2 receptors, making it the only terpene that functions like a cannabinoid. These terpenes may explain why whole-plant cannabis products often outperform isolated cannabinoids for pain conditions.
Best consumption methods for migraine relief
Not all consumption methods work equally well for migraines. Timing is everything when a migraine is building, and some delivery methods are simply too slow to catch it.
Inhalation (vaping or smoking) provides the fastest relief, typically within 2 to 5 minutes. This makes it the preferred method for acute migraines that are already in progress. The 2019 Journal of Pain study found that inhaled cannabis was the most effective delivery method for reducing migraine severity in the moment. If you use a quality vaporizer, you avoid the combustion byproducts of smoking while still getting rapid onset.
Sublingual tinctures and oils are the middle ground. Effects typically begin within 15 to 30 minutes, and the dosing is much more precise than inhalation. Full-spectrum CBD oils may be particularly useful for preventive treatment because they contain multiple cannabinoids that work together. Many migraine patients report taking a consistent daily dose of CBD oil to reduce the frequency of attacks over time.
Edibles are less practical for acute migraine attacks because they take 30 minutes to 2 hours to kick in. However, they offer the longest duration of effect (4 to 8 hours), which can be useful for multi-day migraine episodes. If you tend to get migraines that last 24 hours or more, a combination approach of inhalation for immediate relief followed by an edible for sustained effect may work well.
Topicals applied to the temples and neck can provide localized relief without psychoactive effects. Research from the European Pharmaceutical Review has documented transdermal CBD’s ability to reduce localized inflammation and pain. Some migraine patients swear by CBD balms applied to the temples and back of the neck at the first sign of an aura.
💡 Pro tip
Keep a fast-acting option like a vape pen or sublingual tincture on hand for acute attacks, and use a daily CBD regimen for prevention. Many patients report the best results with this two-pronged approach.
Dosing guidelines for cannabis migraines
Dosing cannabis for migraines isn’t one-size-fits-all, and getting it wrong can actually make headaches worse. The relationship between cannabinoids and migraine pain follows what pharmacologists call a biphasic dose-response curve: low to moderate doses tend to reduce pain, while high doses can sometimes intensify it.
For THC, most clinical studies that showed positive results used doses in the range of 2.5 to 10 mg. Starting at the lower end makes sense, especially if you don’t use cannabis regularly. The Harvard Health guidelines for medical cannabis recommend starting with 2.5 mg of THC and waiting at least two hours before taking more.
For CBD, the dosing range is wider. Studies on cannabis and pain conditions have used anywhere from 15 mg to 150 mg daily. For migraine prevention, many practitioners recommend starting with 25 mg of CBD per day and gradually increasing over several weeks. The World Health Organization’s review of CBD found it to be generally well-tolerated even at higher doses.
A combination of THC and CBD may be more effective than either alone. The 2017 study presented at the 3rd Congress of the European Academy of Neurology found that a 200 mg daily dose of a THC:CBD combination reduced migraine attacks by 40.4%, outperforming a traditional tricyclic antidepressant (amitriptyline) used for migraine prevention.
📝 Important note
Start low and go slow. Cannabis overuse headache (also called medication overuse headache or rebound headache) is possible with daily high-dose THC use. The same phenomenon occurs with triptans and NSAIDs. Keeping your THC doses moderate and taking periodic breaks can help prevent this.
Cannabis strains and profiles for migraines
Strain selection matters for migraines, but not in the oversimplified “indica for pain, sativa for energy” way that many dispensaries still promote. What actually matters is the cannabinoid and terpene profile. The Frontiers in Neurology journal has published research showing that specific terpene combinations influence pain outcomes more than the indica/sativa distinction.
For acute migraine relief, look for strains high in myrcene and beta-caryophyllene with a moderate THC content (15-20%). These terpenes have analgesic properties and the moderate THC level provides pain relief without the cognitive impairment that comes with high-THC strains. Strains like OG Kush, Harlequin, and ACDC are commonly recommended in medical cannabis programs for migraine patients.
For preventive use, high-CBD strains with a CBD:THC ratio of at least 2:1 tend to work best. These provide the anti-inflammatory benefits of CBD while keeping psychoactive effects minimal. If you need to function during the day, a CBD-dominant product like those available from broad-spectrum CBD oils lets you maintain your daily dose without any impairment.
Some patients who experience migraines with aura report that low-dose THC taken during the aura phase can prevent the headache from developing fully. This is anecdotal but consistent with what we know about THC’s effect on cortical spreading depression, the neurological event believed to cause migraine aura, as documented by the American Migraine Foundation.
Potential risks and side effects
Cannabis isn’t a risk-free option, and being honest about the downsides matters. The most common side effects reported in migraine studies include dry mouth, dizziness, and fatigue. These tend to be mild compared to the side effects of prescription migraine medications, but they’re worth knowing about.
The tolerance issue flagged in the 2019 Journal of Pain study is real. Patients who used inhaled cannabis regularly needed higher doses over time to achieve the same level of relief. This mirrors what happens with traditional migraine medications and is something to discuss with a healthcare provider. Periodic tolerance breaks can help reset your sensitivity.
There’s also a paradox worth mentioning: while cannabis can treat migraines, cannabis withdrawal can trigger them. Regular users who abruptly stop may experience rebound headaches, according to data from the CDC’s cannabis health effects page. Tapering off gradually rather than stopping cold turkey can minimize this risk.
If you take other medications for migraines, potential interactions exist. CBD is known to inhibit certain cytochrome P450 enzymes, according to FDA research, which means it could affect how your body metabolizes other drugs. Always tell your doctor about cannabis use if you’re on prescription medications.
How to start using cannabis for migraines
If you’re considering cannabis for migraine management, a structured approach will get you better results than trial and error. Here’s a practical framework based on what the research and clinical experience suggest.
First, keep a migraine diary for at least two weeks before starting cannabis. Track your migraine frequency, intensity (on a 1-10 scale), duration, and any triggers you notice. This gives you a baseline to measure against. Several mobile apps like Migraine Buddy make this straightforward.
Second, choose your approach. For prevention, start with 25 mg of CBD daily, ideally as a sublingual oil taken in the morning. Monitor for four to six weeks before adjusting. For acute attacks, have an inhalation option ready. A small portable vaporizer with a strain you’ve already tested in a non-migraine state is ideal.
Third, track your results carefully. After each migraine (or lack thereof), note what you used, the dose, the timing, and the outcome. This data becomes invaluable over time. Many patients discover specific patterns, like finding that cannabis works better when taken at the first sign of aura rather than after the headache has fully developed.
Finally, work with a healthcare provider who understands cannabis medicine. Organizations like the Society of Cannabis Clinicians maintain directories of physicians trained in cannabinoid therapeutics. A knowledgeable provider can help you optimize your approach and avoid interactions with other medications.
Frequently asked questions
Can CBD alone help with migraines, or do I need THC?
CBD alone can help, particularly for prevention. The anti-inflammatory and FAAH-inhibiting properties of CBD address some of the underlying mechanisms of migraines. However, the strongest clinical results have come from products containing both THC and CBD. For acute attacks, THC’s direct pain-blocking action through CB1 receptors tends to provide faster and more noticeable relief than CBD alone.
How quickly does cannabis relieve a migraine?
It depends on the delivery method. Inhaled cannabis (vaping or smoking) typically provides relief within 2 to 5 minutes. Sublingual tinctures take 15 to 30 minutes. Edibles are the slowest at 30 minutes to 2 hours. For migraines already in progress, inhalation is the most practical option for fast relief.
Will cannabis make my migraine worse?
It’s possible, particularly at high THC doses. Research shows a biphasic response where low to moderate doses reduce pain while high doses may increase sensitivity. Cannabis overuse headache is also documented in regular, heavy users. Start with low doses and track your response carefully. If cannabis consistently worsens your headaches, it may not be the right treatment for you.
Is it safe to use cannabis alongside migraine medications?
CBD inhibits certain liver enzymes (CYP3A4 and CYP2D6) that metabolize many medications, including some triptans and beta-blockers. This means CBD could raise the blood levels of these drugs, potentially increasing side effects. Always consult with your doctor before combining cannabis with prescription medications. THC at low doses is less likely to cause interactions but should still be discussed with your provider.
What cannabis strains are best for migraines?
Focus on the terpene and cannabinoid profile rather than the strain name. For acute relief, look for strains high in myrcene and beta-caryophyllene with moderate THC (15-20%). For prevention, high-CBD strains with a 2:1 or higher CBD:THC ratio work well. ACDC, Harlequin, and OG Kush are commonly recommended. Always check lab results rather than relying on strain names alone, since the same strain can vary significantly between growers.
⚠️ Disclaimer
This article is for informational purposes only and does not constitute medical advice. The information provided about cannabis and migraines is current as of March 2026 but may change as new research emerges. Always consult with qualified healthcare professionals before using cannabis for migraine treatment. Decisions about cannabis use should be made in consultation with healthcare providers who understand your specific medical history and conditions. For our full disclaimer, visit cannastoreams.gr/disclaimer.




